Mucogingival surgery is no longer that difficult today,
procedures have been standardized and great masters spread all over the world aesthetic surgical concepts previously unknown to the vast majority of dentists.
However, there are some really messed up situations where the technical aspects are still very tough and engaging. The treatment plan also requires a bit more attention, but what you really need to be careful with are technical issues… Everyone is good at overthinking and jerking off their brains but those who are actually good at using their hands are much fewer.
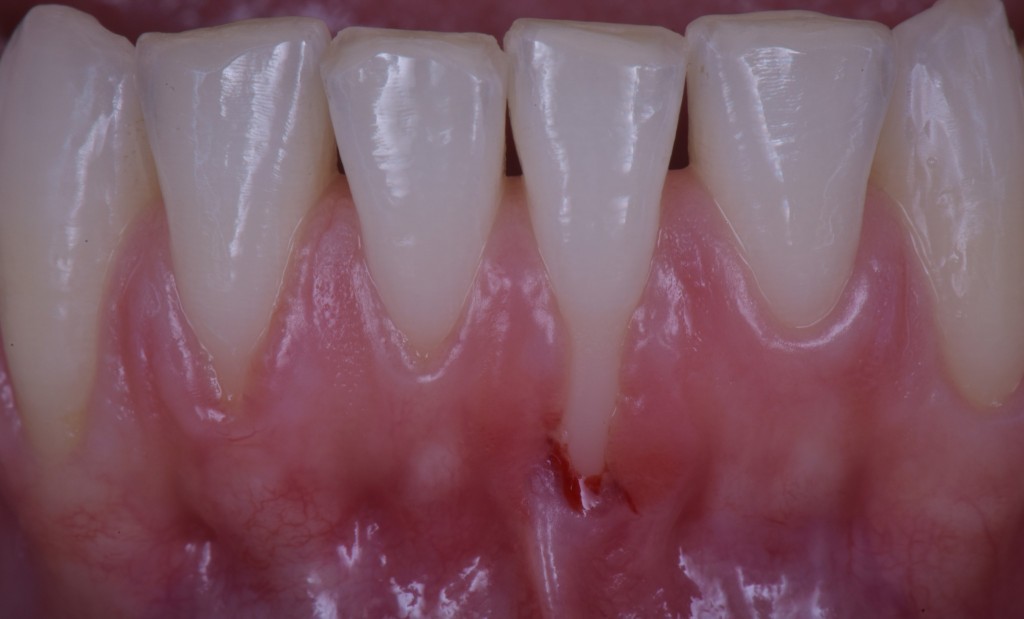
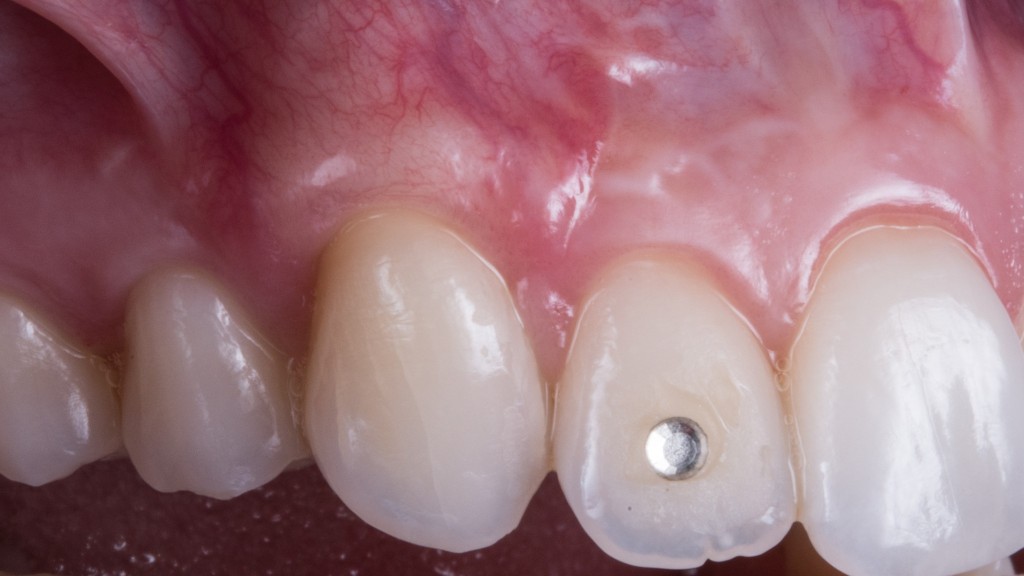
When you have to cover a gingival recession and there is no keratinized tissue, you must take some factors into consideration.
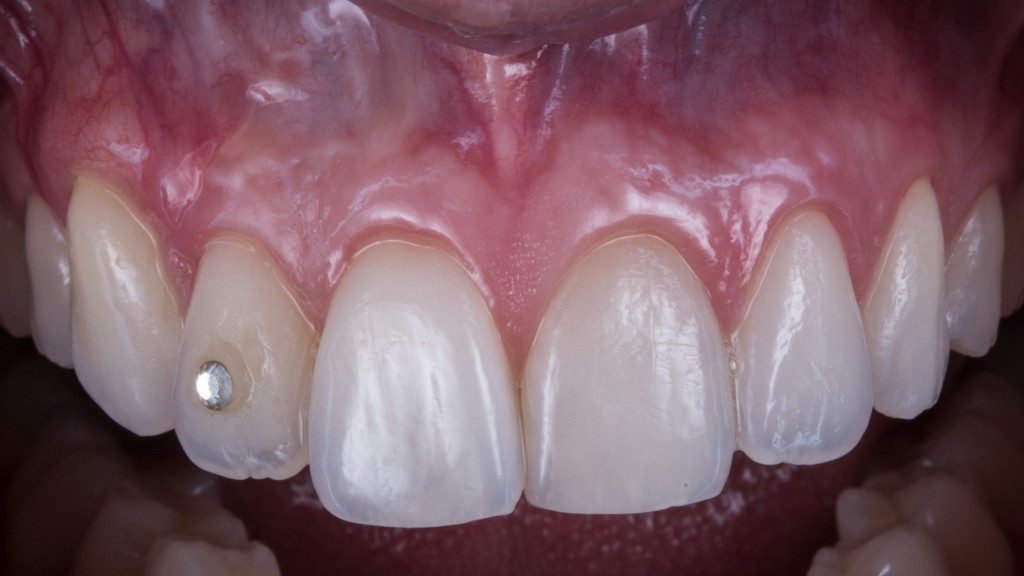
Let’s consider this case as an example. Indication of surgery: 10 out of 10… technical difficulty: 10 out of 10.
That means, this case is a huge problem, but someone has to handle it. You can learn how to do it by yourself, thus getting all your personal fulfilment and the patient’s thankfulness… or you can lose the patient, because someone else will take care of it in your place.
I’d rather learn to do it… what about you?
We have some factors to consider:
- The tissue must be improved in some way. In fact if you cover the recession with that shitty tissue you now have apically, rest assured you will have a relapse. And guess what? You will lose the patient and get tons of complaints on her part. Alice had to get married some months later. I mean… margin of error: ZERO!
- In these cases collagen matrix doesn’t work. You need autologous stuff.
- You can put there new tissue either as a free gingival graft or as a bilaminar connective tissue graft.
Should I be confronted again with such a situation (you can find the video of this case treatment here)
I’d have no doubt. In my opinion the best solution is a double surgery session. I know there are other options, but for me the two-stage treatment (free gingival graft followed by coronally advanced flap) today is the gold standard for this kind of situations!
We get the improvement of the tissue in the first step via a free gingival graft put apical to the recession.
“Why don’t you try to cover the root a little bit with the graft?”
Because if you put the graft over the avascular root surface you will be forced to feed it with a much bigger surrounding recipient site, and, in the end, provided you succeed, guess what?… awful shitty big white stamp!
If you perform a free graft over a vascularized bed, instead, you can do it as little as you want. And, to get the best aesthetic result, we are supposed to do it as wide as the amount of keratinized tissue apical to the adjacent teeth.
Once the graft are re-vascularized we will be able to move it coronally. In this case the graft is pediculated and it will survive even over the avascularized root.
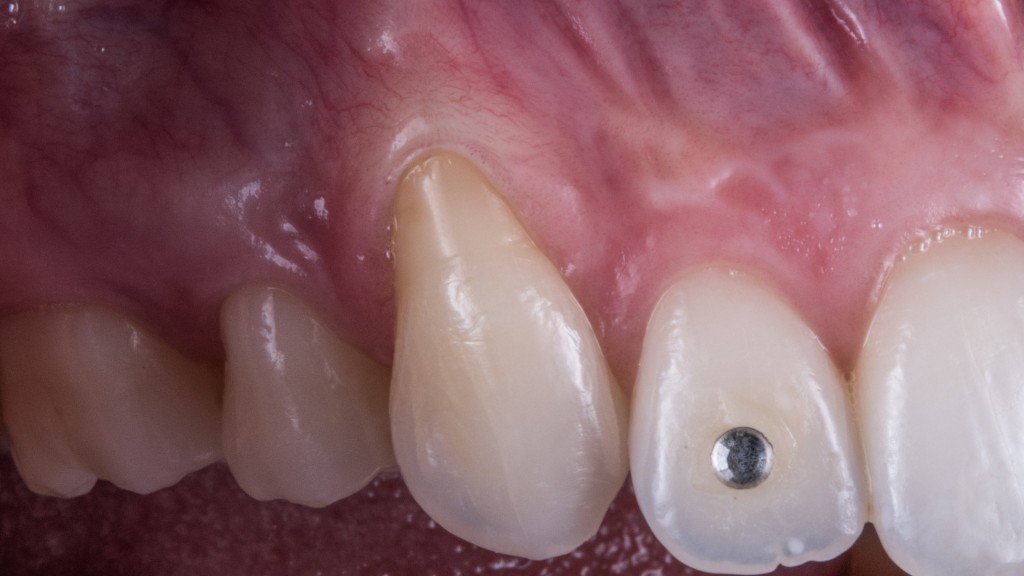
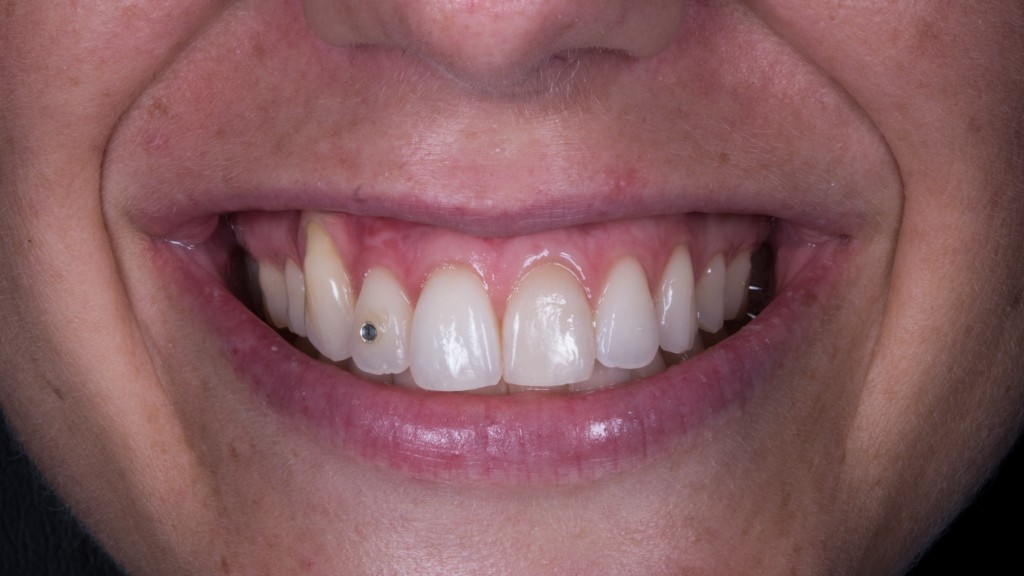
But, as you see, a little bit of “stamp effect” is there anyhow. And Alice wouldn’t have accepted this result on her upper canine!!
So, in upper frontal cases the free gingival graft is forbidden! But we have to improve the tissue at any cost, so the only chance we’re left with is the bilaminar connective tissue graft.
Just let me clarify the concept. Covering the connective tissue graft with alveolar mucosa, the tissue will remain nonkeratinized!
Now you must probably be thinking:
“What a fucking bullshit! Stop playing professor Know-it-all and go back to university!”
Sorry man, but there is a misunderstanding about this concept deriving from the word-of-mouth superficial (and ignorant) transmission of some data from an interesting experiment carried out back in 1978.
Karring et al. grafted some connective tissue (coming from the keratinized gingiva) underneath the epithelium in the fornix of some monkeys. And in that way they have shown the connective tissue drives to the keratinization of the overlaying epithelium…
… unfortunately the word of mouth stops here. Acutally the authors removed the original fornix epithelium some months after graft and only at that time the new keratinized tissue appeared.
So:
- If you cover the palatal connective tissue with the alveolar mucosa, the tissue goes thicker but remains nonkeratinized, i.e. darker.
- If you remove the original nonkeratinized epithelium (or the graft gets exposed by itself because our surgery sucks) you will get palatal keratinized tissue. And you will get the unwanted dreadful white stamp effect!
As you can see in this case, we don’t have a perfect top-notch solution. We must reach a compromise:
PALATAL STAMP
Or
NONKERATINIZED TISSUE WHICH COVERS A STRONG TISSUE OF THE RIGHT THICKNESS
In mandibular cases, I myself choose the first option, in the maxilla I always opt for the second one.
But remember: there are 4 fundamental aspects you have to take into account when managing such a case! Let’s discover them in the video.
Don’t forget to subscribe to the newsletter! And to take a look at my online course, which is full of useful tips and tricks!
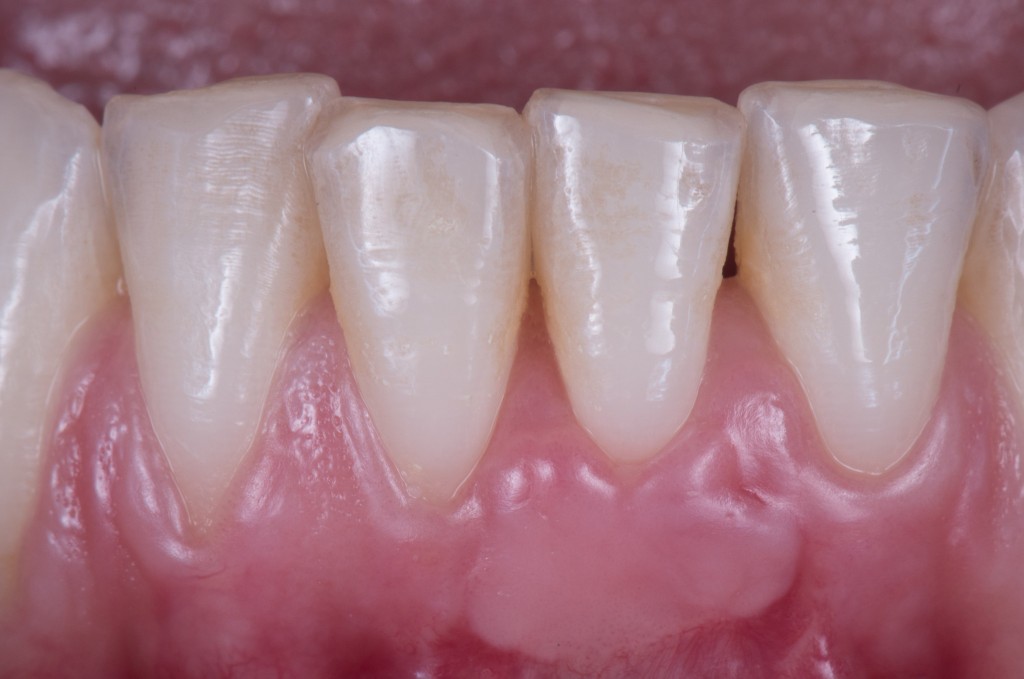
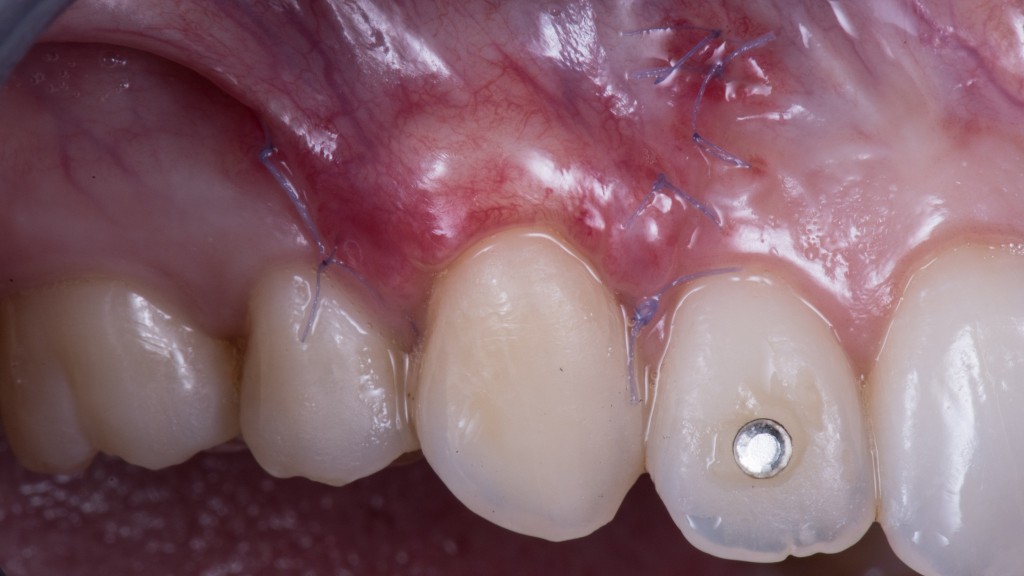
Doh! I was about to forget the 15th day healing pic (as you know it is the critical one!).
And also a pic of Alice!
And also a photo of Alice and I!!… She is a dental hygienist!