There’s a new problem in dentistry that will knock you out of the game in no time if you don’t figure out to learn a few things.
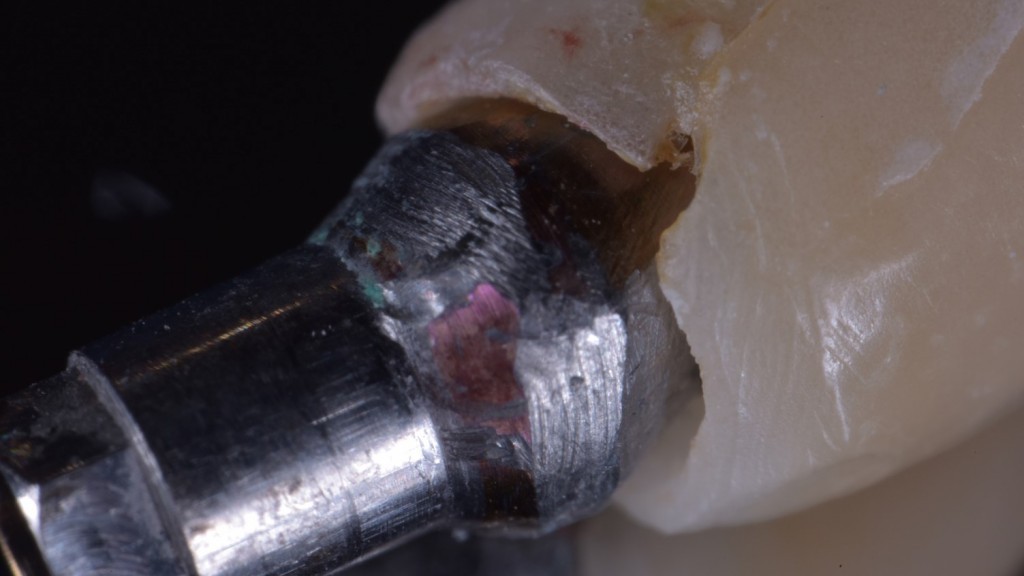
This problem’s name is peri-implantitis. In the past, surgeons used to place very few implants, and everything was done very carefully, on selected patients. Today, however, everyone deserves an implant, all surgeons put them, buying the cheapest ones and competing with each other using the least possible sterilized setting to prove that they’re cool and it works anyway. And they put the most crazy things on it… look here what I have to unscrew from an implant put by a “colleague” a few months ago…
And obviously they don’t do any periodontal preparation because the patient has no money and “it’s already a lot if he can pay for the screw!”
All this leads to peri-implantitis percentages that after 5 years are well over 10%.
Peri-implantitis is often not symptomatic so the patient is not aware of anything and since most colleagues don’t schedule periodic checks on patients and don’t make regular x-rays and probing on implants (although I am quite sure that’s not your or my case)…
…Bam! Peri-implantitis goes on and destroys the basal bone in a way that we didn’t see so often in the past, causing vertical bone defects and precluding the possibility to put new implants in an easy way.
So we have a large number of patients that:
- Are used to implants;
- Would never ever think to talk about a partial removable denture;
- Maybe don’t have posterior natural abatements for fixed bridges;
- Often they are pretty pissed off at the previous dentist who didn’t tell him anything about peri-implantitis getting worse;
- Even more often they are rather sceptical;
- And they don’t have enough bone or keratinized tissue to put new implants.
But there’s more! After all you might say “even years ago it happened to find patients with severe atrophy and I don’t think many dentists have gone off the market”.
You’re right, in fact in the past there were two elements:
- There were a small percentage of very serious atrophy and it wasn’t a big problem for honest dentists to leave them to more experienced professionals. Today severe vertical defects are beginning to affect a significant part of our patient stock.
- People were uninformed and it was very easy for dishonest dentists to tell the patient that in “your case WE REALLY CAN’T PUT IMPLANTS because the gum is not strong enough”.
Today, AT LEAST (!!!!!!!!), and this is the second “problem”, the explosion of health information and advertising, especially thanks to the web, has made the population much more aware of what are the real possibilities in surgery.
And if you ever think to use the old technique of “HERE WE REALLY CAN’T” with good probability you would see the patient leave for other shores where he would find a surgeon able to regenerate the bone vertically and put the implants successfully.
Possible outcome:
- You lose the patient;
- You lose the patient’s family;
- You lose all your cherished word of mouth from that patient and his family who instantly move on to the new hero of modern implantology that solved his problem.
OMG, what a tragic scenario! So what’s the solution?
Well, here it is the solution: you have to learn how to regenerate the bone vertically in order to be able to treat in your practice all these new challenging cases resulting from peri-implantitis damage. Trust me, they’ll be more and more!
And don’t believe anyone who tells you that you need magic hands. It’s all bullshit!
All you need is the right concepts and the right preparation. We’re talking about nailing a membrane and stretching two flaps to close them on! Not carving the Michelangelos’ Pietà from a block of marble!
In addition to concepts and preparation, however, there is another thing that is essential to get started:
TRUST.
After all, if you don’t believe in what can happen under a non-absorbable barrier … well, it will be very difficult for you to invest your time and precious money to learn these techniques that “only a few know”!
So here’s the meaning of this post, to show you, with a piece of video taken from a live surgery of my last advanced implant surgery course, what happens under a PTFE membrane after nine months.
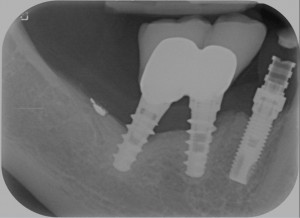
This was the initial situation of the case:
After removal, there was only 5 mm left before the nerve. Minus the safety 2mm, it makes 3mm and, as far as I know, there are no 3mm implants and even if there were, I wouldn’t use them to treat a previous failure!
Now I’ll leave you to the video, and turn up the volume, you have to hear the sound!
See ya!